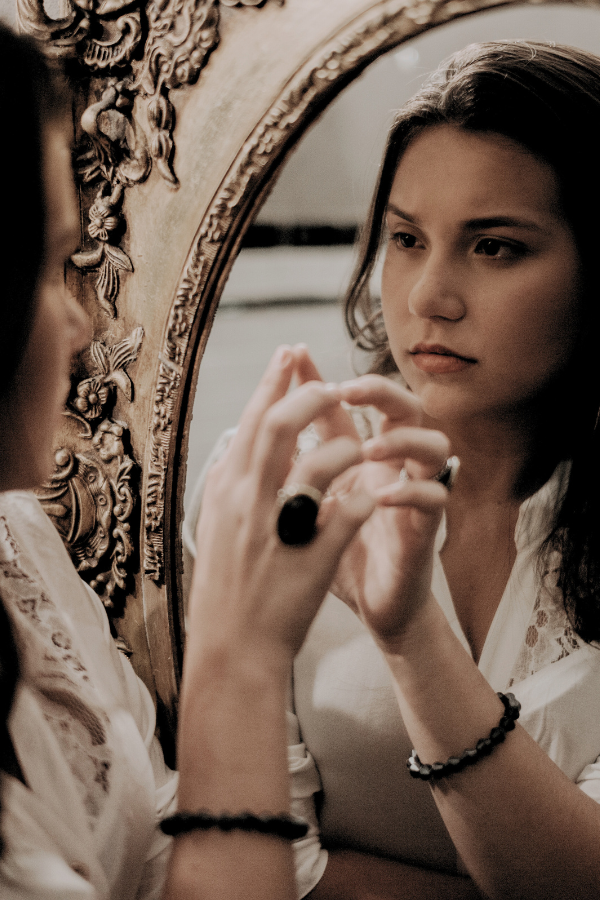Nutritional Psychiatry: The Link Between Diet and Mental Health
Summary
Reflection Questions
Journal Prompt
Nutritional psychiatry and nutritional psychology are predicated on the idea that food, far from being merely sustenance, plays a pivotal role in shaping both our physical and mental health. This innovative approach seeks to understand and harness the therapeutic potential of dietary interventions to complement traditional psychiatric treatments, thereby opening new avenues for managing mental health disorders. By integrating dietary strategies into mental health treatment plans, it addresses the biological underpinnings of mental health conditions, which could reduce reliance on medication, mitigate side effects, and provide a more accessible form of intervention for many individuals. Read on to learn more about the science behind nutritional psychiatry and the diet-mental health relationship.
Historical Context for Nutritional Psychiatry


Historically, the connection between diet and mental health has been acknowledged, albeit in a less scientifically rigorous context. Ancient civilizations, such as the Greeks and Romans, intuitively recognized the importance of diet in maintaining both physical and mental well-being, prescribing various foodstuffs for their mood-altering properties.
However, it wasn’t until the advent of modern scientific methods that researchers began to systematically explore the biochemical links between what we eat and how we feel. This exploration has revealed a complex network of interactions, suggesting that dietary patterns directly impact mental health through mechanisms such as inflammation, oxidative stress, and the gut-brain axis.
The hypothesis that dietary patterns can influence mental health is gaining empirical support, with a growing body of research indicating that diets rich in fruits, vegetables, fish, and whole grains are associated with reduced risk of depression and anxiety, whereas diets high in processed and sugary foods are linked to an increased risk of these conditions. This relationship underscores the importance of considering diet as a key component of mental health and wellness, and it serves as the foundation for the field of nutritional psychiatry.
The Science Behind Nutritional Psychiatry


The gut-brain axis represents a complex communication network linking the enteric nervous system of the gastrointestinal tract with the central nervous system. This bidirectional pathway is not only pivotal for maintaining gastrointestinal health but also plays a significant role in influencing brain function and mood.
The mechanism involves neurotransmitters, hormones, and immune system factors that are produced in the gut and can affect brain health. Microbes in the gut, for example, can produce neurotransmitters like serotonin and dopamine, which are critical for mood regulation. This connection underscores the importance of gut health for better mental health outcomes in addition to improved physical health, suggesting that a healthy gut microbiota may support optimal brain function.
The Role of Nutrients in Brain Function
Nutrients play a crucial role in brain health, impacting various cognitive processes and mood regulation. For example, Omega-3 fatty acids, found in fish oil and certain plant oils, are vital for brain health. They contribute to the fluidity of cell membranes, support neurogenesis, and possess anti-inflammatory properties that are crucial for maintaining cognitive function and may reduce the risk of mood disorders.
Vitamins, minerals, and antioxidants are essential for brain health, supporting neurotransmitter synthesis, providing energy to brain cells, and combating oxidative stress that can damage brain cells. For instance, B vitamins are critical for methylation processes that produce neurotransmitters and energy. Minerals like zinc and magnesium play roles in neurotransmitter activity and neuroprotection. Antioxidants from fruits and vegetables help neutralize free radicals, reducing oxidative stress and potentially lowering the risk of cognitive decline.
The health of the gut microbiota, influenced by probiotics, also has significant implications for mental health. Probiotics can enhance the integrity of the gut barrier, reduce inflammation, and modulate the gut-brain axis. Evidence suggests that probiotics may help improve mood, support mental health, and boost cognitive function, although more research is needed to fully understand their effects on mental health.
Research Findings on Dietary Patterns and Mental Health Outcomes


Rich in fruits, vegetables, whole grains, olive oil, fish, and low in processed and sugary foods, the Mediterranean diet has been associated with a lower risk of depression and anxiety. Its benefits are thought to stem from its high content of nutrients that support brain health, including omega-3 fatty acids, antioxidants, and fiber.
In contrast, diets high in refined sugars and processed foods have been linked to adverse mental health outcomes, including an increased risk of depression and anxiety. These dietary patterns may contribute to inflammation, oxidative stress, and alterations in the gut microbiota, which negatively affect brain health.
Studies in health psychology have found correlations between dietary patterns and the prevalence of mental health disorders. For instance, adherence to healthy dietary patterns like the Mediterranean diet is associated with a reduced risk of developing depression, while a diet high in processed and sugary foods is linked to an increased risk. Let’s take a closer look at recent research findings into food choices and mental wellbeing.
SMILES Trial (2017)
One of the most pivotal studies in nutritional psychiatry is the SMILES trial, which stands for “Supporting the Modification of lifestyle In Lowered Emotional States.” This randomized controlled trial demonstrated that dietary improvements could effectively reduce symptoms of depression. Participants who followed a Mediterranean-style diet for 12 weeks showed significant improvement in depression scores compared to a control group receiving social support alone.
The SUN Project (2018)
The Seguimiento Universidad de Navarra (SUN) Project is a long-term, ongoing cohort study that has provided valuable insights into the impact of the Mediterranean diet on mental health. Findings from the SUN Project suggest that adherence to a Mediterranean diet is associated with a lower risk of developing depression.
NutriNet-Santé Study
This large-scale cohort study conducted by nutritional psychologists in France has explored various aspects of nutrition and health outcomes, including mental health. Research stemming from the NutriNet-Santé Study has highlighted the negative associations between ultra-processed food intake and mental illness, including increased risks of depressive symptoms.
The HELFIMED trial (2019)
The HELFIMED trial focused on the effects of a Mediterranean-style diet on individuals with severe depression. Results indicated improvements in depression scores, quality of life, and overall well-being among participants adhering to the Mediterranean diet, reinforcing the potential of dietary interventions in mental health care.
Examining Specific Nutrients and Their Effects on Mental Health
Omega-3 Fatty Acids


Omega-3 fatty acids, particularly EPA and DHA found in fish oil, play a pivotal role in brain health and have been linked to reductions in symptoms of depression and anxiety. These essential fats are integral components of cell membranes in the brain and are involved in anti-inflammatory pathways and neurotransmitter function.
Recent nutritional science research indicates that omega-3 supplementation can lead to improvements in mood and reductions in the severity of depression, suggesting their potential as an adjunct treatment for these conditions. The anti-inflammatory effects of omega-3s may also underlie their benefits for mental health, as inflammation is increasingly recognized as a pathophysiological mechanism in depression and anxiety disorders.
B Vitamins
B vitamins, including folate (B9), cobalamin (B12), and pyridoxine (B6), are crucial for brain health, playing roles in neurotransmitter synthesis and energy metabolism. Deficiencies in these vitamins have been associated with mood disorders and impaired cognitive function.
B vitamins are involved in methylation processes that regulate gene expression and the synthesis of neurotransmitters such as serotonin and dopamine, which are directly linked to mood regulation. Supplementation with B vitamins has shown promise in improving mood and cognitive function, highlighting their importance in mental health and well-being.
Vitamin D


Vitamin D, often referred to as the “sunshine vitamin,” has a significant impact on mood disorders and cognitive performance. Low levels of vitamin D have been associated with an increased risk of depression, suggesting a potential role for vitamin D supplementation in preventing or treating depressive symptoms.
The exact mechanisms by which vitamin D influences brain function are still being explored but may involve the regulation of neurotrophic factors and neurotransmitters, modulation of the immune system, and neuroprotection. Given the widespread prevalence of vitamin D deficiency, especially in colder climates with less sunlight exposure, addressing vitamin D levels could be a key strategy in improving mental health outcomes.
Magnesium, Zinc, and Iron
Magnesium, zinc, and iron are trace minerals essential for numerous physiological processes, including those critical for brain function and mental health. Magnesium plays a role in neurotransmitter release and protection against excitotoxicity, with supplementation shown to have anxiolytic effects. Zinc influences neurotransmitter function and is essential for neurogenesis; its deficiency has been linked to mood disturbances.
Iron is crucial for oxygen transport and energy metabolism in the brain; iron deficiency, especially in early life, can have long-lasting effects on cognitive development and mood. Adequate intake of these minerals through diet or supplementation may support mental health by ensuring the proper functioning of biological processes critical for mood regulation and cognitive performance.
Dietary Patterns and Mental Health Disorders


The relationship between dietary patterns and mental health disorders is an area of growing interest and research. The Western diet, characterized by high consumption of red meat, processed foods, sugary desserts, and refined grains, has been linked to an increased risk of developing mental health disorders such as depression and anxiety.
In contrast, the Mediterranean diet, which emphasizes the intake of fruits, vegetables, whole grains, fish, and olive oil, has been associated with lower rates of these disorders. This contrast highlights the potential impact of diet on mental health, suggesting that the quality and types of foods consumed can influence brain health and emotional well-being.
The Mediterranean diet’s rich content of anti-inflammatory and antioxidant components, along with omega-3 fatty acids, might contribute to its protective effects against mental health disorders by reducing inflammation and oxidative stress, factors that are implicated in the pathophysiology of depression and anxiety.
Evidence from Epidemiological Studies and Clinical Trials on Diet Modifications and Mental Health Outcomes
Epidemiological studies and clinical trials have provided compelling evidence linking diet modifications to mental health outcomes. For instance, longitudinal studies have shown that adherence to healthy dietary patterns, like the Mediterranean diet, is inversely associated with the risk of developing depression. Furthermore, randomized controlled trials (RCTs) have demonstrated that dietary interventions, such as increasing the intake of nutrients rich in omega-3 fatty acids or following a Mediterranean dietary pattern, can lead to improvements in symptoms of depression and anxiety.
These findings are supported by the SMILES trial, which is among the first RCTs to directly examine the effect of dietary improvement on major depressive disorders. The trial found that participants who followed a modified Mediterranean diet experienced significant improvements in depression symptoms compared to a control group. Such evidence underscores the potential of dietary modifications as a cost-effective, accessible, and natural adjunct therapy for improving mental health outcomes, highlighting the critical role of diet in the prevention and management of mental health disorders.
Practical Applications of Nutritional Psychiatry


Incorporating the principles of nutritional psychiatry into daily life involves understanding and applying the connection between diet and mental health. Start by emphasizing whole foods rich in nutrients known to benefit brain health, such as omega-3 fatty acids, antioxidants, vitamins, and minerals. These are abundantly found in fruits, vegetables, lean proteins, whole grains, and healthy fats like those from fish, nuts, and olive oil.
Planning meals that incorporate these foods, reducing the intake of processed and high-sugar foods, and staying hydrated can significantly impact one’s mental well-being. It’s also beneficial to maintain regular meal times, which can help stabilize mood and energy levels throughout the day. Mindful eating practices, such as paying attention to hunger and fullness signals, can further enhance the relationship with food and its impact on mood.
Dietary Recommendations for Improving Mental Health Outcomes
Dietary recommendations for improving mental health outcomes emphasize a balanced intake of nutrients that support brain function. The Mediterranean diet is often highlighted for its mental health benefits, promoting the consumption of fruits, vegetables, whole grains, legumes, nuts, seeds, fish, and olive oil, while limiting red meat, processed foods, and sugar.
Adequate intake of omega-3 fatty acids, found in certain foods like salmon, mackerel, and sardines, is crucial for brain health. Incorporating a variety of colorful fruits and vegetables ensures a wide range of antioxidants and phytochemicals, which protect the brain from oxidative stress. Ensuring sufficient dietary intake of vitamins B, D, and minerals such as magnesium, zinc, and iron can also support mood regulation and cognitive functions.
Challenges and Considerations in Implementing Dietary Changes for Mental Health Improvement
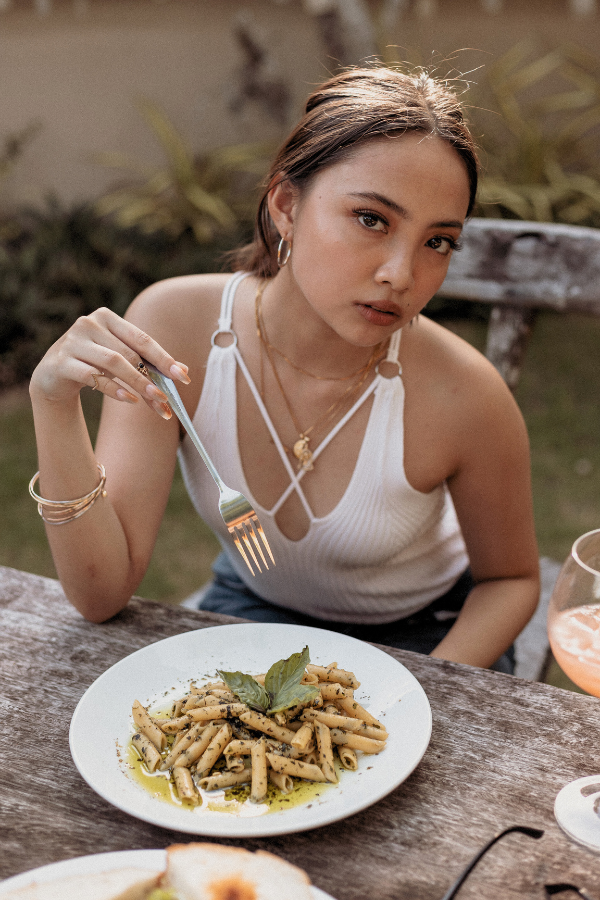
Implementing dietary changes for mental health improvement can present several challenges and considerations. One of the primary hurdles is the accessibility and affordability of healthy food options, particularly in areas with limited availability of fresh produce and whole foods. Personal preferences, dietary restrictions, and cultural food practices also play significant roles in shaping one’s diet and can complicate the adoption of new eating habits.
Overcoming habits of consuming processed and convenience foods requires not only motivation but also education on healthier alternatives. Additionally, it’s important to recognize that dietary changes should complement, not replace, traditional psychiatric treatments. Achieving a balance that respects individual needs and conditions is crucial for the success of integrating dietary interventions for mental health improvement.
The Essential Role of Healthcare Professionals in Integrating Nutritional Advice with Traditional Psychiatric Treatments
Healthcare professionals play a critical role in integrating nutritional advice with traditional psychiatric treatments. We recommend that those considering major changes to their diet for health reasons consult with a nutritional psychologist or certified nutritionist. By adopting a holistic approach to mental health care, professionals can address both the biological and psychological aspects of mental disorders. Psychiatrists, psychologists, and therapists can collaborate with dietitians and nutritionists to develop comprehensive treatment plans that include dietary interventions alongside medication and therapy.
Healthcare providers should be informed about the latest research in nutritional psychiatry to offer evidence-based dietary recommendations. Training in nutritional psychiatry principles can enhance their ability to support patients in making dietary changes that may improve mental health outcomes. This multidisciplinary approach underscores the importance of considering diet as a component of mental health treatment and the value of healthcare professionals in guiding patients through the process.
Final Thoughts on Nutritional Psychology: Dietary Habits and Mental Health


The potential of nutritional psychiatry lies in its ability to offer non-invasive, accessible interventions that can be tailored to individual needs and preferences. This approach does not suggest replacing current psychiatric treatments but rather enhancing them, providing a multi-faceted strategy for managing and preventing mental health issues. By integrating dietary modifications—emphasizing nutrient-rich foods, balanced intake of essential vitamins and minerals, and reducing processed food consumption—individuals can support their mental health alongside traditional therapeutic and pharmacological interventions.